Aquagenic urticaria (also called aquatic pruritus, allergic to water, aquatitis hives, or aquagenous urticaria) is a subset of physical urticaria. This type of hives develops after contact with water on the skin. This may include activities such as bathing, sweating, swimming, rainy weather, and other similar activities in which water comes into direct contact with the outer skin (epidermis).
Although it is often described as a “water allergy,” it is usually not classified as a true allergy by doctors or researchers, and is instead grouped as one of the physical urticaria subtypes. It tends to be less common than other forms of physical urticaria, such as dermatographic urticaria. It may develop at any age, but most physical urticaria subsets develop most commonly during the late teens or early 20’s.
A common misconception is that since the body is made up of significant amounts of water, and since water is a necessity for human life, it is impossible to be truly allergic to water. Therefore, some people may be skeptical of the claims of those suffering with water urticaria. Some even ask the question: “Can you be allergic to water?”
In reality, individuals with aquagenic urticaria do indeed experience a hypersensitive response in the skin after direct stimulation or contact with water substances. This can be very painful, itchy, or embarrassing for the individuals, and they can live with the condition for years without being diagnosed for fear of rejection or embarrassment.
Although people suffering from water urticaria can usually drink water safely, they may experience reactions around the mouth if the water contacts the external skin when drinking.
Aquagenic Urticaria Symptoms
Aquagenic urticaria symptoms are similar to other forms of physical urticaria. Symptoms can include intense itching (pruritus), burning sensation, small raises hives or wheals, and flushing of the skin in the areas that come into contact with water. These symptoms usually appear within minutes after exposure to a water substance, although rarely the reaction could be delayed by a few hours.
Once the skin is no longer in contact with water, the hives will gradually subside. In many cases, the hives and wheals will disappear within only a few minutes. Occasionally, the hives may persist for a few hours after the initial reaction (which is known as “delayed onset urticaria”), although this is not quite as common.
Aquagenic Urticaria Causes
Doctors aren’t sure exactly what causes aquagenic urticaria. It has been speculated by some doctors and researchers that this condition may develop due to a hypersensitive immune system in the skin reacting to one of several stimuli. Some of the hypotheses include:
- Sensitivities to chemical additives in the water (such as chlorine, hard water, and other chemicals).
- Weakened mast cells in the skin that react to the sensation of water
While researchers do not yet know the exact cause of aquagenic hives, they do know that the itching, flushing, burning, and other related sypmtoms are due to the release of histamine. When histamine is released, the chemical reacts with the surrounding tissues causing the itching and burning sensation., as well as raised wheals or flushing.
Aquagenic Urticaria Diagnosis
Aquagenic urticaria is usually diagnosed by a dermatologist or allergy specialist. It may also be diagnosed by a general physician with familiarity of physical urticaria. In most settings, a doctor will simply examine the skin and place water on it to observe the reaction. If the water causes a hypersensitive reaction in the skin (hives, itching, wheals, etc), then it could be an indication of water urticaria.
Doctors may perform routine blood-work or other tests to rule out more serious conditions or diseases. Also, it is not unusual for people suffering with water allergy to have a history of other allergy or hives.
Aquagenic Urticaria Treatment (Or Cure)
Although there is no known cure for aquagenic urticaria, there are some treatments which may help alleviate symptoms. Some of these treatments include:
- Antihistamines–Antihistamines can help lessen the severity of the itching, burning, and redness that occurs during a reaction. In severe cases, doctors may use higher doses, or combine different types of antihistamines to achieve a reduction in symptoms (such as combining an H1 and H2 antihistamine).
- Mast Cell Stabilizers–Medications that help stabilize and strengthen mast cells can also be useful for some cases of urticaria.
- Water Filtration and Avoidance–Minimizing water contact on the skin is a way to avoid reactions. This includes wearing appropriate clothing to prevent sweating, brief showers, and more. In addition, using a water filter or water softener may help remove chemicals in the water.
- UV therapy–In some cases of urticaria, UV therapy has proven useful. This can be costly for some, and may include side effects of the skin such as increased skin cancer risks.
- Vitamins & Diet Modifications–For some urticaria conditions, it is also useful to remove any foods which increase allergic responses. Low histamine diets and restricted diets of known food sensitivities may be recommended. Avoiding common allergens such as wheat, dairy, eggs, and others may be useful. In addition, some individuals with urticaria may have low levels of vitamin d and other vitamins. Check with a doctor for a simple blood test that can determine any vitamin deficiencies.
- Hypoallergenic Products–It may also be useful to use hypoallergenic soaps, shampoos, detergents, and more. Also, avoiding external allergies (such as pollen, pet hair, dust mites, etc.) may help lessen symptoms.
To see what helps others with this condition, visit our forum.
Aquagenic Urticaria Pictures & Images:
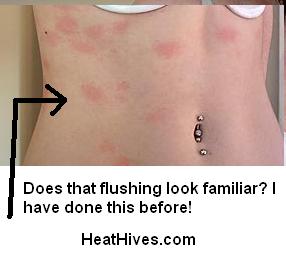
As you can see from the image below, aquagenic urticaria leaves flushing and red blotches. Some individuals may develop small pinpoint hives, raised wheals, and extreme itching (that feels like a sting or tiny bug bites). This reaction often subsides within a few minutes once water is removed from the skin. Urticaria symptoms often differ from person to person. Some individuals may experience very little itching or burning, and may only experience redness. Others may have few visible symptoms, but may feel extreme itching and stinging. These can vary significantly for each person, like many other urticarias.